Birth Story: Arabella's Vaginal Breech Birth at St James's University Hospital, Leeds
- Charlotte Watson
- Apr 8, 2022
- 10 min read
Updated: Feb 4

They (the doctors and midwives) commented afterwards that my room was the calmest on the floor that night.
From Terrified to Exited with Hypnobirthing - what a transformation!
In the early stages of pregnancy with my first daughter I felt terrified about the prospect of giving birth. Fortunately, I’d also heard about hypnobirthing and positive birthing experiences people who had practised hypnobirthing in pregnancy had. I booked a private one-to-one course and at 20 weeks my husband, Martin, and I went along. Martin didn’t have a clue what I had signed us up for, but he was fully supportive, exactly what I needed. After the first session I felt such a transformation, from initially being terrified about birthing my baby, I left the session feeling excited to give birth, what a turnaround! The reason for this change, was realising despite the name sounding a bit airy-fairy, hypnobirthing was actually really scientific and evidence based. From the course I could understand how my mind, body and baby worked together during labour and birth and this gave me so much confidence. I also realised I had choices about how and where I birthed my baby which was empowering. This, along with understanding how I could build a relaxation toolkit and use decision making skills all helped me feel calmer and more confident for my baby's birth.
Discovering baby in breech position
My pregnancy was relatively straightforward and at the 20-week scan appointment, my daughter was positioned in a Frank Breech position with her bottom towards my pelvis with her legs extended up in front of her face. A position she quite comfortably remained in until birth.
FYI, a baby being bottom down at 20-weeks doesn’t mean the baby will be breech at term (40+ weeks), there is still plenty of space and time for the baby to rotate head down, and sometimes babies will rotate in labour. A baby presenting breech at term is rare, about 4%, sometimes breech is described as “the wrong way round”, although it can also be referred to as “a variation of normal”.
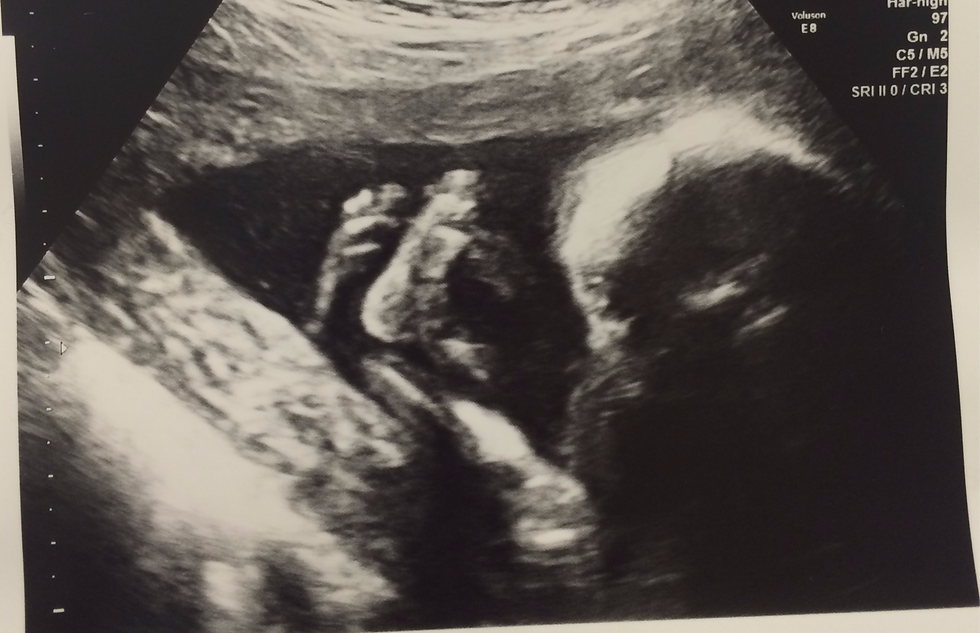
Assessing my options with a breech baby with information and support
As my pregnancy progressed, my daughter appeared to be very comfortable in her streamlined bum down legs up position and it became more apparent that maybe she might need a little encouragement to rotate head down. During this time, I read up on my options for birth, talked to my health care team, including my midwife and obstetrician, all to help me work out what felt least stressful for me and my baby. My options appeared to be a planned caesarean section birth or spontaneous vaginal birth.
I found the Breech Birth UK Facebook group hugely helpful as it enabled me to talk to other mothers who had experienced a similar situation and asses my options, talking to them about their experiences. I also found the Spinning Babies website an excellent source of information, I burnt Moxibustion sticks and laid upside down on my ironing board to encourage her to turn, but she was apparently quite comfortable and happy how she was and maintained her breech position.
Trying to rotate baby with an External Cephalic Version (ECV)
I also had an External Cephalic Version (ECV) at Leeds General Infirmary hospital (LGI) at 38+3 weeks. During this procedure I was given a muscle relaxing drug and baby was monitored via an ultrasound while the obstetrician used her hands on my belly to manually manipulate my baby to turn head down. The ECV was an uncomfortable procedure, but listening to my hypnobirthing tracks and focusing on my breathing really helped. After 20 minutes of trying, the obstetrician said she had been able to rotate my daughter head down, but when she moved her hand away, my daughter flipped straight back. The doctor said I was coping very well and she could keep trying, or see if another obstetrician might be able to try, which I declined. I had been hopeful it would work, but I understood ECV success rate was 50%.
I felt deflated and emotional after the unsuccessful ECV. For me the thought of a planned surgery was more stressful than a spontaneous labour. I had an open, unbiased, conversation with the obstetrician about my options and she gave me the benefits and risks of both caesarean section and vaginal birth, then gave me a week to think about my options, which I appreciated.
Labour starts spontaneously:
“that was the calmest voicemail you’ve ever left, hypnobirthing obviously works" - Martin
It appeared my daughter knew what she wanted and at 39+1 weeks; 2 days before my next consultant appointment, my waters broke at home. I’d woken up from a nap around 4pm and went to the loo, I then felt the need to go to the loo again, and again, finally realised my waters had released in a trickle, and I was not in fact wetting myself! Thank goodness!
I felt calm and excited! My contractions started about an hour later. I started timing them and called the midwife who asked me to go to the hospital. I had planned to go to Leeds General Infirmary (LGI) however it was too busy so I was asked to go to St James’ University Hospital (Jimmy’s) instead. As my baby was breech, I understood once I was in hospital I wouldn’t be sent home until she was born. I also understood increasing my oxytocin levels would help labour progress and didn’t feel any urgency to rush in so I made myself some pasta to eat (carb loading!), downloaded some funny films onto my iPad, to get the oxytocin and endorphins flowing, and printed off my birth preferences (which I hadn’t actually finished writing – I’d recommend being a little more organised if possible!) I called Martin at work and left a voicemail, he said to me later “that was the calmest voicemail you’ve ever left, hypnobirthing obviously works”. He came home from work and after another couple of hours at home timing contractions and a hearty meal, we headed to the hospital.
"Am I doing the right thing?"
Walking into St James (Jimmy's) Hospital I had a wobble, I suddenly wondered if I was doing the right thing opting for a vaginal birth as my plan A. Martin calmly reassured me that I was informed and this is what felt right for me and our baby, I needed to hear that. We arrived in the Maternity Assessment Centre (MAC) and the midwife performed a vaginal examination (VE) to check my cervical dilation, I remember constantly apologising to her that I was leaking fluid everywhere and making a mess! She was lovely, of course. A registrar then did an ultrasound scan to check the fluid level and confirm baby’s position was still breech, which it was. Following the scan, she advised in this situation they would recommend a caesarean section. I said I had discussed the options with the consultant, I understood my birth might evolve into an unplanned caesarean (plan B) and I was most comfortable to proceed with a vaginal birth as my plan A. The registrar then recommended epidural pain relief which I also said I didn’t want as a first option and she replied “you seem very well informed, good luck” and left us to it.

Remaining active in labour
During my pregnancy I had remained active, walking a minimum 4 miles a day to and from work as well as regularly swimming and doing pilates. Early labour was no different, I stayed as mobile as possible, walking around the hospital grounds and in time moved to a more private room which I made my own, ensuring it was dark and putting on my playlist. As labour progressed the midwives advised continuous monitoring of my baby, which I agreed to, so I was attached to a cardiotocography (CTG) machine and laid on a bed on my back. I had a maximum of 3 contractions laid on my back and they were so painful; my whole body shook. I didn’t stay laid on my back much longer. I got off the bed and was instantly more comfortable, my contractions didn’t take over my whole body when I was upright. However, being upright meant the CTG machine was unable clearly trace the contractions, but I refused to be laid down to accommodate for the machine. Martin was also tracking the contractions on his phone and the midwives ended up following his track rather than the CTG machine.
Moving to the delivery room
After a while I consented to another VE (which wasn’t wholly comfortable as I had to lie on my back again) and my cervix was 7cm dilated. After this I was then transferred to a delivery suite room. For a while a student midwife held the CTG monitor so it could get a reading and I could remain active as I wanted. I will forever be grateful to this midwife for supporting me in the ways I needed at that time. I then changed to having wireless monitoring meaning I could be more active and mobile. I made the room my safe space again, making it dark and playing my music. I used the bed to lean over while I sat on a birth ball and Martin did a soft touch massage. I had some paracetamol for pain relief, although I’m not 100% sure it did anything and I also used gas and air, but it made me vomit and I think it threw off my breathing, I was blowing out instead of inhaling the gas and biting hard on the mouthpiece instead of having a relaxed jaw.
"I wouldn’t describe my birth as easy, it was work, it took effort, the sensations were intense... but the hypnobirthing techniques helped me to remain calm and manage well."
Hello Baby Girl
When it was time to give birth to my daughter, I had moved on the bed, on all fours this time, leaning over the raised head of the bed. I felt the pushing urge and went with it. The midwife told me my baby was moving down but she kept moving back up the birth canal. I was reaching a stinging point and didn’t want to push any further, the midwife told me I needed to push through the stinging pain to get her down and she would stop going back up. There was a point before she was born where I suddenly felt scared, like I couldn’t do it anymore, I was filled with fear and doubt, I was tired and I wondered why I hadn’t opted for a caesarean birth as my first option. Then I remembered this was completely normal, I had been taught about this in my hypnobirthing course. This fear was a normal surge of adrenaline and meant I would soon be meeting my baby. Martin was right next to me and I was holding his hand, a little too tight, he might say. I pushed my baby down and out. She was born bum first, while I was kneeling on the bed. There was a little time between contractions to birth her head while she sat like a little buddha on the bed. The doctors then helped me turn over to my back and with the next contraction her head was born, at 39+2 weeks gestation, 3:41am at the start of a lovely summer day, weighing 6lb 14oz. My daughter was handed to me for skin-to-skin contact, and I said to Martin “It’s Arabella!” She was beautiful, I was so proud, I had done it, we had done it together, she was here! We were a family!

After she was born she was checked over by the doctors and she was perfectly healthy. The midwife then said I needed to birth the placenta. A bit of me thought “What! Are you kidding, I just birthed a human! no more” but it was fine. I had skin to skin with Arabella, minimal blood loss and no need for an oxytocin injection. The midwife checked to see where the placenta was, it appeared Arabella had been wearing it like a hat, as her head was covered in blood, and with another contraction I pushed out the placenta. The beautiful organ that had nourished my baby during her time inside me. The midwife then checked for any tears, and I was fortunate to have only a graze, meaning no stitches and maybe doing that perineum massage in late pregnancy had paid off.
Reflecting on my vaginal breech birth experience
Reflecting on my vaginal breech birth, I can honestly say I had a positive birth experience. I wouldn’t describe my birth as easy, it was work, it took effort, the sensations were intense. There were points I questioned whether having a surgical caesarean birth would have been easier. However, the hypnobirthing techniques helped me to remain calm, much of that came from getting informed, practising my relaxation toolkit before birth. Hypnobirthing also gave Martin a focus on how to effectively support me during birth, as well as during pregnancy when I was making informed decisions. I practised and put in the work before birth, it gave me confidence in my body's ability and in trusting myself and my own instinct. I was fully supported by my care team, including two midwives, a student midwife and two doctors (an obstetrician for me and a paediatrician for Arabella – just in case).
The health care team commented afterwards that my room was the calmest on the floor that night. I knew I had established my route of least stress, that my birth may evolve into a plan B (caesarean birth) and I was comfortable with that. As it was, plan A seemed to work just fine for Arabella and I. My post birth recovery was good, I suspect easier and quicker than if I had had a caesarean section.
For some, a planned surgical birth is the least stressful, and therefore best option, for others a spontaneous onset of labour is, it is about looking at your individual situation, getting informed and working out what is best for you and your baby and feeling supported in that decision.
Hypnobirthing changed my life
I loved hypnobirthing and my birth so much, in 2021 I retrained and qualified as a Hypnobirthing teacher, and in 2024 as a Doula, offering nurturing support and evidence based information to families during their own pregnancy and birth journeys.
I can help you get informed and feel confident, relaxed and empowered for your baby's birth.
I offer birth and postnatal doula support alongside a variety of Hypnobirthing antenatal courses and Birth Prep Power Hour sessions.
Visit the Positive Birth Leeds website for the latest group or private course information or book a FREE discovery call to have a chat through what support best suits your needs.
Charlotte x
If you want more information for Breech presenting babies, I have attached some links here for you:




Comments